Development and exploration of a new model for understanding depression
Michael Gathercole
Defining of depression
Causative Models of Depression
A New Model for Depression
Overview of Treatment Approaches
References
Reproduced with the author's permission. This paper was published in The Australian Journal of Counselling Psychology, Volume 5, Number 4, 2004, pp 7 - 17.
Abstract
This paper presents a model of depression that is an elaboration of the currently dominant 'biopsychosocial' model.
Details are presented to demonstrate that much research has been conducted into possible explanations of depression and, as a consequence, many potential factors have been identified. However to the present time there has been a lack of clarity about how the underlying mechanisms for depression may work.
In addition to attributed numerous possible causes, almost as many treatments have been postulated. It will be shown that whilst some of these approaches are reasonably effective, no treatment so far has proven to be universally so. What is more confusing is that a significant number of the treatment approaches are moderately effective but have quite dissimilar explanatory frameworks. In addition, clear links between theory and treatment are often tenuous.
After defining depression, I briefly summarize the research literature in terms of causative evidence and explore some of the models that have been generated to explain these results. Particular attention is given to the adequacy of the models to account for research evidence. A new integrative model, developed in part by the author, is then described. After presenting this model major treatment approaches are described within the framework of this model.
Defining Depression
'Depression' is characterized by feelings of helplessness, hopelessness, inadequacy, and sadness. However these are symptoms of several disorders and can also occur in normal individuals (Wolman 1973). A clinical diagnosis of depression has to be accompanied by a range of other symptoms of certain duration. These include: a loss of interest or pleasure in life, significant diet changes, sleep disturbance (most commonly insomnia), psychomotor changes, decreased energy and tiredness, a sense of worthlessness and an impaired ability to concentrate and make decisions (American Psychiatric Association 2000).
While some cultural differences about the expression and frequency of depression have been observed, depression seems to occur in all cultures (Kleinman and Cohen 1997). As well as cultural differences in the rate of occurrence, the frequency of depression also changes over time within specific cultural milieux. For instance, since the Second World War, the reported rate of depression has been steadily increasing around the world. In Australia, the rate of occurrence for the diagnosis of depression has increased threefold. It is now the most common mental health diagnosis and it is expected to be the third major contributor to years of life lost by 2016 (Mclntyre 1999).
DSM-IV-TR Categories
In the DSM-IV-TR, mood disorders with depression are broken into unipolar and bipolar depressions. The model discussed in this paper relates to the much more common spectrum of unipolar disorders. These include major depressive disorder, dsythmic disorder and depressive disorder not otherwise specified (American Psychiatric Association 2000).
There is some debate in the literature concerning the validity of the existence of the three categories of unipolar depressions. Beutler, Clarkin et al. (2000) argue that it might be equally valid to conceptualise the three unipolar disorders as representing different degrees of severity of one psychological phenomenon (Beutler, Clarkin et al. 2000).
Summary of Research Findings on Causal Factors
Strong empirical evidence exists for possible causal factors in four broad domains; namely biological, developmental, skills based and context. It is worth noting, however, that much of the discussed research is primarily correlational in nature, so causality is not always conclusively established.
Biological Factors Relating to Depression
A large range of different biological factors has been established as being commonly present in those suffering from depression. This includes genes, hormones, light, personality and certain disease states.
Genetic Factors
The evidence for a genetic influence is especially strong, particularly for the more severe forms of depression. Monozygotic twin studies have shown that concordance with bipolar disorders is 80% and severe unipolar 59%. Heritability for more minor forms of depressions has however not been as clearly established (Nurberger and Gerson 1992).
Given that these concordance figures are not absolute, even for bipolar disorders, they indicate that genes are more likely to lead to vulnerability to develop a depressive disorder, under certain environmental conditions, rather than the development of a specific depressive condition. It is also clear that any genetic influence that does exist is multigenic in its origin, thereby indicating that genetic vulnerability will vary along a continuum. That is, the greater the loading on certain genes, the higher the biological vulnerability (Ratay and Johnson 1997).
Whilst there is probably a genetic component to most presentations of depression, these cannot be the whole explanation for the condition. The rate of depression has been demonstrated to fluctuate greatly over time and from country to country (Beutler, Clarkin et al. 2000). Clearly, any possible genes responsible for depression could not mutate so quickly (Hamer and Copeland 1998).
Hormonal Factors
Hormonal factors outside the obvious mood related hormones and neurotransmitters have also frequently been linked to depression and there is little doubt that they play a role in some depressive episodes, particularly postnatal depression (Yapko 1994). There have, however, been some exaggerated claims for the impact of hormones on depression. For example female hormones have been used as an explanation for the observation that women have a rate of depression twice that of men in the West. Behavioural and cultural explanations for those observed gender differences are more probable as there is clear evidence that some cultures, such as some pacific islanders, do not experience any gender difference in the rate of depression and for some it is more prevalent in men (Brannon 1999).
External Agents and Medical Conditions
A number of external agents and medical conditions have also been linked with depression. These external agents include a lack of sunshine, a number of medications, including some illicit and legal drugs, viruses and chemicals in the environment (both natural and synthetic). Some medical conditions such as MS are also claimed to have an associated high rate of depression, well beyond that associated with similarly debilitating conditions (Beutler, Clarkin et al. 2000).
In summary, many biological factors have been linked to the occurrence of depression. Although a biological vulnerability may actually need to be present for depression to occur, its expression as depression in most cases is far from absolute. The level of vulnerability so generated is also quite variable. At present, in keeping with the biological focus in psychiatry, genetic, hormonal and pharmacological factors are receiving the greatest attention in regard to both the causes and treatment of depression.
Adverse Developmental Events
Many early negative life events have been found to be associated with depression in adolescence and adulthood. Specifically, there is very strong evidence of a relationship between a lack of adequate parental care in childhood and the expression of depression in adulthood (Parker 1992). Major trauma or loss in childhood has also been effectively linked to depression, even in old age (Kivela, Luukmen et al. 1998).
As for biological explanations, the direction of causality is reasonably well established concerning such adverse developmental events and depression. Extreme adverse events of childhood, such as sustained neglect or abuse have even been shown to cause structural brain changes, primarily in the limbic system and prefrontal cortex. The reversibility of such damage is still highly contested (Teicher 2002). Less extreme abuse can cause similar changes in some children but others seem to show a natural resilience (Ciarrochi, Chan et al. 2001).
It is worth noting that depression is not the only possible consequence of such adverse developmental events. They seem also to increase vulnerability to many other mental illnesses, such as anxiety, schizophrenia and personality disorders (Teicher 2002). The one expressed is probably dependent on underlying biological vulnerabilities and possibly later life events.
In summary, adverse developmental events have an established causal relationship with depression and seem to increase vulnerability by forming structural detrimental changes in the brain. As for biological vulnerability, the extent of developmental vulnerability generated by adverse events is quite variable.
Coping Skills Deficit Factors
There is some disagreement in the literature on what makes someone resilient. Models tend to divide around aspects of what a person is versus what they do (Carpenter 1992). Given that innate factors have been addressed in terms of the biological domain, the latter focus will be adopted here. To make the distinction clear, I will use the phrase "coping skill deficit" rather than just "coping deficit". Coping skills can be categorized in terms of whether they are behavioural, cognitive, emotion and/or body-based.
Behavioural Coping Skills
A range of behavioural coping skills has been clearly associated with positive mental health, while their absence has been associated with depression. These skills include behaviours such as rational action, perseverance, restraint, self-adaptation, seeking help and open expression of feelings to name a few (McCrae 1992).
Cognitive Coping Skills
In regard to the cognitive domain, the presence of significant cognitive distortions has been linked with depression, most particularly in regard to negative perceptions of self, one's future and the world in general (Beckham, Leber et al. 1986).
The absence of cognitive distortions is also strongly associated with positive mental health as is the use of a range of cognitive strategies such as reframing and learnt optimism (Seligman 1994).
Affect Related Coping Skills
Affect related coping skills are largely dependent on a person's emotional intelligence. Emotional intelligence is the ability to perceive, understand, express and manage emotions (Ciarrochi, Chan et al. 2001).
Abilities in regard to emotional intelligence are strongly linked with immunity from depression and other positive mental health outcomes. Whilst probably having a genetic component, this quality seems to be more amenable to learning than general intelligence. Improvements in these areas are possible with proper coaching and have been shown to reduce depression when achieved (Greenberg 2002).
Body Awareness
Changes in body sensation and posture have long been associated with depression. These changes are often associated with low body awareness. Changing awareness of the body can, of itself, change these states and relieve symptoms of depression (Kurtz 1990).
Proviso for Coping Skill Discussions
Concerning the area of coping skills in general, it needs to be noted that it is hard to be certain how much the observed absence of coping skills is a product rather than a cause of the depression. Prolonged depression in and of itself reduces a person's coping skills repertoire, particularly cognitive skills. In addition, simply not doing something for more than six months greatly erodes the skill base. This phenomenon has been well demonstrated in the context of individuals, including prisoners who have recently been released from long stays in residential facilities (Crosby 1987). One of the hallmarks of a depressed person is apathy and a lack of action, which would reduce coping skills over time.
Some longitudinal studies however have been performed that indicate a tendency to pre-existing coping skill deficits in those who develop depression (Carpenter 1992).
Negative Contextual Factors
Contextual factors are the current life events and circumstances that buffet an individual. When negative in nature they have long been posited to link to depression. In fact, the hypothesized connection is almost as old as civilization itself and was referred to in some of the very first Greek medical treatises (Porter 1997).
More recent efforts have tried to identify salient events. There seem to be at least three main ones linked to depression, namely grief and loss, existential factors and life stressors. The following sections will elaborate further on these.
Grief and Loss - Related Contextual Factors
The relationship between grief, loss, sadness and depression has been known since ancient times and is the aspect of depression most consistent with lay perceptions of the disorder and one that is clearly self-evident. It is worth noting that nearly all non-cyclic depressive episodes do have some precipitating loss event that can be identified (Payhel and Cooper 1992).
Having said that, the very nature of depression makes recall of negative events stronger and may exaggerate the strength of this relationship. Strong memories always have an emotional component and are easier to recall when again in that emotional state. Specifically, when you are sad it is much easier to recall previous sad life experiences (LeDoux 1998).
Existential Contextual Factors
Existential contextual factors refer to the extent that the environment generates a sense of belonging and personal meaning for the people living in it; or in terms of depression a lack of these things. Many depressed people experience a sense of disengagement and lack of meaning in their lives. Such experiences are one of the criteria for a diagnosis of depression (American Psychiatric Association 2000).
The locus of control for the inner felt sense of disengagement and meaninglessness may be either internally or externally based. Internal factors include the presence of faulty negative cognitions and a negative view of self and the environment, which relates more to the coping skills deficits discussed earlier. Alternatively, an external toxic environment may provide low rates of positive reinforcement and/or high rates of punishment for an individual and result in feelings of depression. However, without an objective evaluation of the environment, it is very difficult to distinguish between the internal and external factors, particularly when both factors may be operating at the same time to some extent (Gilbert 1992).
Contextual Stressors
Individual stress is generally defined in terms of external and internal factors. Cohen et al (1995) for example defined stress as occurring when "environmental demands exceed the adaptive capacity of an organism, resulting in [adverse] psychological and biological changes" (p3). Many of the internal or adaptive factors were of course discussed above. The focus here, instead, is on the other side of the ledger.
The significance of environmental and social [contextual] factors to the generation of stress in individuals was first recognized back in the 1930s. Efforts to systematically measure these factors however did not commence until much later. The first such checklist measure, introduced in 1957, was the Schedule of Recent Experiences (SRE). Since then many other scales have been produced and a plethora of studies have been undertaken to address this issue. Importantly, it is now well established that the more stressful the life events experienced by an individual, the more likely he or she is to experience aversive stress responses such as depression (Turner and Wheaton 1995).
Definitions of contextual stressors usually include experiences of loss, threat and challenge (McCrae 1992). Given that experiences of loss was considered previously, the primary focus here is on environmental experiences of threat and challenge. Some factors that can induce these responses include direct stresses from familial, social and work pressures, indirect stresses from the presence of other mental/physical illnesses and from resent traumatic experiences. Let us briefly expand on each of these in turn.
Much higher levels of family, social and work related stresses are reported by individuals prior to the onset of depression, than nondepressed individuals in the general community. This evidence is based on both self-report assessments and feedback given by relatives and significant others (Payhel and Cooper 1992). Families can also generate another form of contextual stress, in terms of particular family members serving as role models for depressive coping strategies and/or in terms of generating situations that will increase the likelihood of a depressive reaction. Not surprisingly, depression is frequently an intergenerational problem (Yapko 1999).
Concerning other mental and physical illnesses, depression is often considered the "Rome" of health problems, since so many other conditions seem lead to it or are least comorbid with it. Whilst some of these conditions may have a direct biological impact on the occurrence of depression, for most of these associations the illness would primarily appear to be as a contextual stressor, particularly when pain is a component of the condition (Harris 1999).
In addition, many of the so-called symptoms of depression can, themselves, be precursors to depression and therefore act as contextual stressors; this includes psychomotor change, such as a forced reduction in activity level (Parker and Brotchie 1996) and sleep disturbances, such as insomnia (Dement 1999). Certain, qualities of the environment have also been shown to make contextual stressors even more potent, such as the lack of controllability, the chronicity and the severity of the stressor (McCrae 1992). These factors, it needs to be noted, also feed into the severity of existential contextual factors.
In summary, a number of contextual factors (around grief and loss, existential and stress dimensions) have been linked to the presence of depression, although causality has not clearly been established in all cases. It is also self evident that the degree of environmental toxicity experienced by different individuals will vary enormously.
Causative Models of Depression
Although many models exist for the cause of depression, these can be broken into three broad categories. Namely: single deterministic factor models, multiple condition deterministic models and multiple interactive causative models. Each of these categories will now be considered in turn.
Single Deterministic Models of Depression
Initially, most models of the cause of depression were single deterministic models, such as the biological, developmental or contextual model. Whilst statistically significant correlations have been established for many of the individual factors in these models, no one model has provided superior explanatory or predictive power as compared to the others (Freedman, Kaplan et al. 1976).
Multiple Condition Deterministic Models
Whilst a cluster of specific symptoms defines depression, many have realized that this does not mean that it has to be a single illness with a single cause. In fact, it has been recognized for some time that depression probably has multiple causes (Beutler, Clarkin et al. 2000). This understanding can lead to two broad kinds of approaches to models. One is to divide depression into different types by causes, the other to see depression as a product of the interplay of different causes.
The first approach of trying to divide depression into different types dependent on causes is quite old. The best known would be the exogenous versus endogenous model of depression. Some models however have incorporated up to 35 forms of depression (Beutler, Clarkin etal. 2000).
Some subcategories of depression probably do legitimately exist, so this approach is not entirely without merit. Clearly Bipolar Disorders seem distinct disorders and seasonally acquired and postnatal depression may prove to be, so this continuity-discontinuity debate is likely to continue.
In general however, such models have proven to be equally unsatisfactory as the single deterministic models. Whilst some clustering of causative factors occurs, there is also a very high level of overlap of so-called different causative factors within individuals; that is, many people present with more than one clear cause to their depression. In addition, excluding the previously mentioned exceptions, treatment is largely independent of specific sub-category diagnosis (Beutler, Clarkin et al. 2000).
Multiple Causative Models
The last approach is to view depression as being primarily a singular condition caused by a complex interplay of different factors. The best-known model of this type would be the bio-psycho-social model of depression (Clark, Beck et al. 1999). Whilst popular and the best match for available data, such models tend to be used more for theoretical understanding than as a guide for clinical practice.
This is because such models tend to be broadly descriptive with neither the logic between parts of the model clear nor the direction of individual treatment obvious. Such looseness makes for limited usefulness in a treatment context. It was this limitation that led to efforts at my workplace to try and refine the bio-psycho-social model into a clinical practice model. It was felt that it was worth tackling the problem even in a modest fashion due to the potential gains.
A New Model for Depression
Drawing together the research findings discussed earlier and combining them with data obtained from interviews with patients and clinical experience has led to the following bio-psycho-social model of depression. It is hoped that the comprehensive nature of the model will prove to be useful to both practitioners and researchers.
The model first posits that depression is primarily the result of an interplay between individual vulnerabilities and environmental toxicity. Both of these aspects are further differentiated into a number of separate components. The vulnerabilities into biological, developmental and coping skills based; the environmental toxicity into loss related, existential related and context related stress. These divisions were selected to be similar to those mentioned earlier in the literature review.
Individual Vulnerability
The three vulnerability related factors interact to increase an individual's risk of depression. The higher the level of combined vulnerability, the less toxic a given environment needs to be to tip someone over into depression. The model does not assume a greater importance for any of the threes sources of vulnerability. It does however argue for the presence of at least some vulnerability in at least one of the components for depression to occur. Without that, it is postulated that another mental health consequence is likely to result from environmental toxicity.
Whilst individual vulnerability has been broken into three factors, the model acknowledges the interplay between them in producing an overall level of vulnerability. In addition, the sum is assumed to be greater than the parts. Interventions in this domain would largely focus on reducing vulnerability in the component/s identified with issues.
Environmental Toxicity
Each of the three factors of environmental toxicity relate to the contextual dimensions identified earlier from the literature. The greater the toxicity of a given environment, the less vulnerability to depression a person requires to actually display depression. Certain environments would therefore generate much higher levels of depression than others. The model however does not assume that environmental toxicity is always a necessary causal component of depression. For some individuals, it is possible that their vulnerability is so great that none may be required.
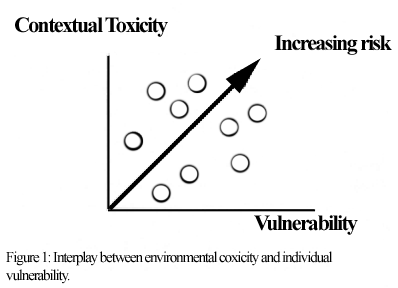 As for vulnerability, the three environmental toxicity factors are acknowledged to interplay with one another. Interventions in this domain may focus on changing the environment or working through the consequences. The interplay between all these factors is graphically represented in figure 1.
As for vulnerability, the three environmental toxicity factors are acknowledged to interplay with one another. Interventions in this domain may focus on changing the environment or working through the consequences. The interplay between all these factors is graphically represented in figure 1.
The Threshold Concept
In this model, there is an assumption that clinical depression occurs when an individual's vulnerabilities and level of environmental toxicity combine to reach a certain threshold. The greater the individual's combined vulnerability the lower the level of environmental toxicity required to reach that critical threshold. For some individuals, no environmental toxicity may be required to trip them into depression. For individuals at the other extreme, with very low vulnerabilities, only the most toxic of environments would lead to depression. For most such individuals, depression would be a highly unlikely occurrence.
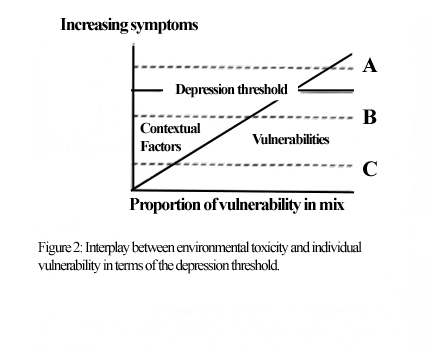 Figure 2 illustrates this interplay between vulnerabilities and the toxicity in the environment. The y-axis indicates the severity of symptoms with the horizontal line representing the threshold for clinical depression. The first dotted line (A) represents someone clinically depressed, the second (B) someone sub-clinically depressed (that is someone with a number of the symptoms of depression but not sufficient for a diagnosis of depression) and the third one (C) someone unlikely to have depressive features. Movements along the x-axis illustrate an increasing extent of the vulnerability component in the mix of an individual's combination of vulnerability and environmental toxicity in their observed presentation.
Figure 2 illustrates this interplay between vulnerabilities and the toxicity in the environment. The y-axis indicates the severity of symptoms with the horizontal line representing the threshold for clinical depression. The first dotted line (A) represents someone clinically depressed, the second (B) someone sub-clinically depressed (that is someone with a number of the symptoms of depression but not sufficient for a diagnosis of depression) and the third one (C) someone unlikely to have depressive features. Movements along the x-axis illustrate an increasing extent of the vulnerability component in the mix of an individual's combination of vulnerability and environmental toxicity in their observed presentation.
The model assumes that continuity exists between the experience of depression and sadness and that the separation is one of degree rather than being absolute. There is some substantial evidence supporting this assumption. Such shadow syndromes or tails of declining distress in symptoms also seem to exist for most other serious mental illnesses (Ratay and Johnson 1997).
Individual Differences
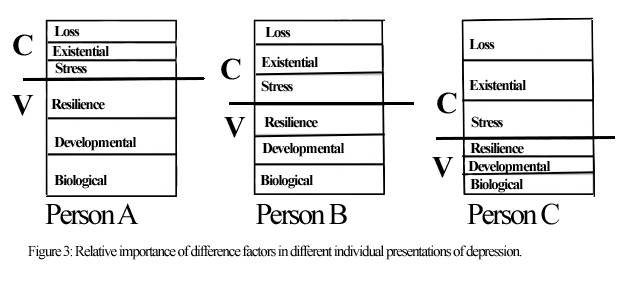
The model postulates that an individual not only differs in terms of his or her overall vulnerability and the toxicity of the environment they are in, but also in terms of the relative importance of each of the vulnerability and environmental components that exist. For some, all six may be very important. In other cases it may just be one. For example, in one individual, personal vulnerability may not be particularly important in his or her depression presentation; for such a person, it might be the losses experienced and existential dimensions that are largely responsible for their depression. In someone else however, it might be biological or developmental vulnerability that is most prominent. Figure 3 shows some possible combinations in this regard to simply illustrate the extent of individual differences possible.
Explaining the Observed Changes in the Rates of Depression
This model permits a researcher or clinician to postulate a range of possible explanations for the observed increase in depression mentioned in the opening section. Broadly these divide into changes in terms of vulnerabilities or contextual factors. In terms of vulnerability factors, people's capacities to cope could be declining (i.e. we have fewer coping skills and are not as resilient as our ancestors were) or the rate of abuse and traumatic events experienced by children could be increasing. In regard to contextual factors, the environment could simply be becoming more toxic (i.e. the world a nastier place than it once was) and thereby increasing the generation of negative changes, disconnection and stress.
Treatment of Depression
This model contains the implication that single treatment approaches to all individuals with depression would be inadequate. The task of the therapist using this model would be to identify a client's unique profile and then determine the appropriate mix of interventions suited to that person.
The overall outcome of a positive result from various interventions often masks the common reality of all therapeutic interventions, that is the fact that some clients gain a great deal, others little and some are actually harmed by the approach. In this regard, the key question isn't which approach is best but "what treatment, by whom, is most effective for this individual with that specific problem, and under what set of circumstances" (Paul 1967, p. 111). This model attempts to address this reality.
Application of this model to clinical practice would therefore require three factors to be present and true. These are:
(1) The capacity to identify the relative importance of each of the components for a given individual.
(2) The existence of different approaches or techniques that can relate specifically to the areas identified in a persons unique profile.
(3) The existence of some overall treatment benefit in targeting specific treatments for individuals.
Let us consider each of these factors in turn.
Overview of Treatment Approaches
The capacity to measure most of the components included in the model is reasonably well established. There are for example good measures for depression, emotion regulation and depression related cognitive distortions readily available (Fischer and Corcoran 1994). The only component that is difficult to measure is, ironically, the biological one.
There are an enormous variety of treatment approaches to depression and an equally large range of factors that need to be considered in terms of the provision of such treatment. Whilst the following list is not exhaustive, it contains most of the main treatment factors and approaches that have proven efficacy.
Generic Treatment Factors that Influence Depression
A reasonable amount of evidence exists for the efficacy of a range of generic factors for the effective treatment of depression. These include the impact of natural improvement, the placebo effect, treatment non-specifics and the treatment of either co-morbidity factors or underlying symptoms (Hubble, Duncan et al. 1999).
Depression is a condition that untreated often has a significant natural improvement (Beutler, Clarkin et al. 2000). The placebo effect is surprisingly powerful in regard to lifting depression. Brown (1998) conducted a meta-analysis of studies of placebo effect and found that it varied from condition to condition but was very strong in depression. Actions that have been shown to maximize the placebo effect include:
The exercise of effort on the client's behalf to obtain the treatment
An apparently rational reason for why treatment should work (rational within the particular cultural context of the client)
The confidence of the therapist
The expectations created during treatment of the likelihood of a positive outcome
The relative authority of the person providing treatment
The combination of natural improvement plus the strong placebo effect has lead to many spurious treatments to be considered falsely efficacious. What is worse there is some evidence that for some treatments (such as some herbal remedies) the outcomes of taking it are actually worse than no treatment (Dawes 1994). Please note that this not true for the treatments discussed later, which have all had substantive impacts above natural improvement and the placebo effect established.
Non-specifics are also very powerful in regard to treatment outcomes for depression. "Non-specifics" are those therapeutic techniques that are almost universal to all treatment approaches. In particular the therapist joining skills, the therapist's display of client respect and use of warm and open communication styles have all been shown to have significant therapeutic impact on depression (Hubble, Duncan et al. 1999).
Given that depression is often contributed to by other mental illnesses, frequently the treatment of the other condition will reduce the depression as well (Porter 1997). This view is consistent with the contextual dimensions of the model discussed earlier. In a similar sense, treating a range of the apparent symptoms can also be highly effective for depression. Most notably in terms of efficacy are interventions that focus on either sleep disorders (such as insomnia) or reversing psychomotor changes (Dement 1999).
There is some debate about the proportion of treatment effectiveness that can be put down to these generic factors. It is most probable that they account for at least close to half the treatment effectiveness (Hubble, Duncan et al. 1999). There is also a range of client qualities that impact on the likely effectiveness of treatment. Those factors however are outside the scope of this paper.
Treatments with Proven Efficacy
To be consistent with the model presented in this chapter, the treatment approaches will be considered in terms of the factor they appear to primarily operate on. It needs to be noted that many popular interventions also lay claim to being able to impact on more than one specific factor in depression. When this is the case, an effort to acknowledge these other areas will also be made in passing at the start of a section. To avoid repetition, however, an approach will only be highlighted once in the body of the discussion in the area that concerns the most significant association. I will, as before, commence with the vulnerabilities and then move onto the contextually related factors.
Biologically-Based Treatment Approaches
A range of different biological approaches to treatment exists with established efficacy. These include a range of pharmacological interventions, ECT and light therapy.
Pharmacological Approaches
The successful treatment of unipolar depression with anti depressants is well established. These medications however do not cure the depression; they simply lift the symptoms of it and all of them have side effects (Feldman, Meyer et al. 1997).
A large number of herbal remedies have had claims made in regard to effectiveness but most have not been clinically proven. One exception is St John's Wort. This herb however has also been reported to have some serious side effects (Parker, Wong et al. 2001).
Electro Convulsive Shock Treatment (ECT)
ECT has established efficacy in regard to lifting severe depression that has not responded to alternative treatments although it does have serious side effects, including brain damage (Beutler, Clarkin et al. 2000).
Ultra Violet Light Exposure
This can be useful for treating seasonally related depression and is of course cheaper than travelling to a sunny location (although not as much fun) (Beutler, Clarkin et al. 2000). Exposure to ultra violet light does however increase the risk of skin cancer.
Damaged Core Remediation Approaches for Developmentally Induced Vulnerabilities
A number of therapeutic approaches could conceptually fit under this umbrella. The most obvious are the psychodynamic approaches. Many other traditions however now claim to work with this material including emotion focused therapies and CBT.
Psychodynamic Approaches
These approaches focus on developing insight and dealing with maladaptive patterns from the past. The evidence shows that it can be quite useful in regard to treating clients with damaged core issues related to developmental vulnerability, but is very labour intensive (Horowitz 1988).
Coping Skill Deficit Approaches
A large range of approaches has developed to meet psychological vulnerabilities due to coping skill deficits. In terms of behaviour and cognitive issues, Cognitive-Behaviour Therapy (CBT) clearly dominates as the preferred intervention. Proponents also claim to attend to emotional factors, but emotion focused therapies would probably hold a stronger claim. In terms of the somatic dimensions, emotion focused therapies lay some claim, but again it would be the more specifically somatic focused approaches like Hakomi and Yoga that would lay stronger claim. It needs to be noted that trying to tease out precise distinctions could create false dichotomies. It is better to see these therapeutic approaches as having very significant areas of overlap in regard to both focus and clinical effectiveness.
Cognitive Behaviour Therapy (CBT)
A large number of cognitive and behavioural strategies have been found to be effective in the treatment of depression (Clark, Beck et al. 1999). Broadly, these focus on changing maladaptive cognitions or behaviours that either lead to the depression or help perpetuate it. Common techniques include changing cognitive distortions, reframing, identifying and changing underlying schemas, Stress Inoculation, and encouraging physical activity and other changes to routine (Brewin 1996).
Psycho-educational interventions are an additional significant subsection of CBT. This approach assumes that the individual has certain knowledge and skill deficits that have lead to the current depressive state, perpetuate it or have been lost as a consequence of the depressive episode. These approaches include social skills training, communication training, emotion regulation training (e.g. anger management), stress and relaxation training and assertiveness training.
Emotion Focussed Interventions
The focus of these therapeutic theories is on the importance of emotional processes. To intervene, a therapist needs to identify key markers of either emotions or process. In terms of emotion markers Greenberg (2002) for example identified the need to differentiate between primary adaptive and maladaptive emotions, secondary emotions and instrumental emotions (Greenberg 2002).
Process markers, in comparison, indicate a psychological point where a client is demonstrating a readiness for change. Various people in the field have identified a number of different process markers. Elliot (2002) for example has identified ten that have been gleaned from empirical studies (Elliot 2002).
The second major emphasis is on interventions for change. Various approaches have been developed to guide therapy when such markers are identified, such as empathic responding, two-chair work or focusing work (Gendlin 1996).
Body and Somatic Focussed Interventions
Body-centred psychotherapy is a way of using a focus on sensations in the body, together with mindfulness as vehicles for inner exploration and resolution of symptoms.
Body-centred approaches also tend to contain a focus on the appropriate use of braking techniques within the therapy, to contain the level of arousal to one the client's body can manage (Caldwell 1997).
Yoga Therapy
Whilst meditation is generally contraindicated for those suffering from depression, a range of other yoga techniques do appear to have proven effectiveness. These include a combination of certain dynamic postures, breathing practices and diet change. Both detachment and the need to take responsibility for one's actions are also emphasized in Yoga therapy. Fairly extensive research has been conducted into these approaches in both India and Japan where they are used as a common treatment for depression. This research has shown a level of efficacy comparable to Western approaches to the treatment of depression (Saraswati 1983).
Contextual Based Approaches
A range of what could be called contextual based approaches also has well-established efficacy. These include bereavement-focused approaches for those with significant grief and loss in their lives and relational and systemic approaches for working with contextual stressors. In terms of the existential area, many treatment approaches also lay claim.
Bereavement Counselling
Therapeutic focus is on helping the individual bring the loss back to life, articulate the experiences associated with the loss and process some of the emotions. The assumption is that the negative mood is part of a natural process rather than something pathological. Adjustment is notably quicker on those bereaved that receive such intervention (McKissock and McKissock 1998).
Interpersonal/Marital/Family Therapy
These approaches focus on intervening in regard to the systems that a client is part of and the quality of their relationships within those systems. Conceptually, such approaches could be particularly useful in regard to existential and contextual stressor based depressions. In regard to treating child and adolescent depression, a systemic approach is frequently more effective than an individual approach (Beutler, Clarkin et al. 2000).
Table 1 below provides a summary of the various treatments discussed above and the area within the model they seem to impinge on. A major claim refers to the area that the approach seems to predominantly focus on and minor an area they approach also makes claims to.
| VULNERABILITIES |
CONTEXTUAL |
| Intervention |
Biological
vulnerability |
Developmental
vulnerability |
Coping skills
deficits |
|
Contextual
grief and loss |
Existential |
Contextual
stressors |
| Anti-depressant |
* | | | | | | |
| ECT |
* | | | | | | |
| Herbal |
* | | | | | | |
| Psychodynamic |
| ** | | | | * | |
| CBT |
| * | ** | | | * | * |
| EFT |
| * | ** | | * | * | * |
| Body-centred |
| * | ** | | * | * | * |
| Yoga |
| | ** | | | * | * |
| Bereavement |
| | | | ** | * | |
| Relational |
| | | | | * | ** |
| Systemic |
| | | | | * | ** |
* = minor claim
** = major claim
Table 1: Treatment approaches and their primary impact areas.
|
Conclusions
In conclusion, the literature provides support for a large range of possible causative factors in depression, from biological, developmental, skill based deficits, contextual factors such as losses, existential deficits and stressors. This body of evidence strongly supports a bio-psycho-social model for depression. Whilst widely accepted, the nebulousness of existing models seem to have given little direction for treatment development or research. In this paper, a refinement of the biopsychosocial model was presented along with some of the implications for both research and treatment.
References
American Psychiatric Association (2000). Diagnostic and statistical manual of mental disorders. Washington, American Psychiatric Association.
Beckham, E. E., W. R. Leber, et al. (1986). "Development of an instrument to measure Beck's cognitive triad: The cognitive triad inventory." Journal of Consulting and Clinical Psychology 54: 566-567.
Beutler, L. E., J. F. Clarkin, et al. (2000). Guidelines for the systematic treatment of the depressed patient. New York, Oxford University Press.
Brannon, L. (1999). Gender: Psychological perspectives. Boston, Allyn & Bacon.
Brewin, C. R. (1996). "Theoretical foundations of cognitive-behavior therapy for anxiety and depression." Annual review of psychology 47: 33-57.
Brown, W. A. (1998). "The placebo effect." Scientific American 278(1): 68-73.
Caldwell, C. (1997). Getting in touch: the guide to new body-centred therapies. New York, Free Press.
Carpenter, B. N. (1992). Issues and advances in coping research. Personal coping: Theory research and application. B. N. Carpenter. London, Praeger.
Ciarrochi, J., A. Chan, et al. (2001). Measuring emotional intelligence. Emotional intelligence in everyday life: a scientific inquiry. J. Ciarrochi, J. P. Forgas and J. D. Mayer. Philadelphia, Psychology Press: 25-45.
Clark, D. A., A. T. Beck, et al. (1999). Scientific foundation of cognitive theory and therapy of depression. New York, John Wiley & Sons, Inc.
Cohen, S., R. C. Kessler, et al. (1995). Strategies for measuring stress in studies of psychiatric and physical disorders. Measuring stress: a guide for health and social scientists. S. Cohen, R. C. Kessler and L. U. Gordon. New York, Oxford University Press: 3-28.
Crosby, R. L. (1987). "Community care of the chronically ill." Psychosocial Nursing 25(1): 33-37.
Dawes, R. M. (1994). House of cards: psychology and psychotherapy built on myth. New York, The Free Press.
Dement, W. C. (1999). The promise of sleep: the scientific connection between health, happiness and a good night's sleep. London, MacMillan.
Elliot, R. (2002). The Process-Experiential approach to psychotherapy. Toledo: 32.
Feldman, R. S., J. S. Meyer, et al. (1997). Principles of Neuropsychopharmacology. Sunderland, Sinauer Associates.
Fischer, J. and K. Corcoran (1994). Measures for clinical practice: a sourcebook. New York, The Free Press.
Freedman, A. M., H. I. Kaplan, et al. (1976). Modern synopsis of comprehensive textbook of psychiatry III. London, Williams and Wilkins.
Gendlin, E. T. (1996). Focusing-oriented psychotherapy: a manual of the experiential method. New York, The Guilford Press.
Gilbert, P. (1992). Depression: the evolution of powerlessness. East Sussex, Lawrence Erlbaum Associates.
Greenberg, L. S. (2002). Emotion-Focused Therapy. Washington, American Psychological Association.
Hamer, D. and P. Copeland (1998). Living with our genes. London, MacMillan.
Harris, N. L. (1999). "Chronic pain and depression." Australian family physician 28(1): 36-39.
Horowitz, M. J. (1988). Introduction to psychodynamics: a new synthesis. New York, Basic Books.
Hubble, M. A., B. L. Duncan, et al. (1999). The heart and soul of change. Washington, American Psychological Association.
Kivela, S. I., H. Luukinen, et al. (1998). "Early loss of mother or father predicts depression in old age." International journal of geriatric psychiatry 13: 527-530.
Kleinman, A. and A. Cohen (1997). "Psychiatry's global challenge." Scientific American 276(1): 74-77.
Kurtz, R. (1990). Body-centred psychotherapy: the Hakomi method. Mendocino, Life Rhythm.
LeDoux, J. (1998). The emotional brain. London, Weidenfeld & Nicolson.
McCrae, R. R. (1992). Situational determinants of coping. Personal coping: Theory research and application. B. N. Carpenter. London, Praeger: 65-76.
McIntyre, K. (1999). Partnerships for public health: Building a platform for better health in Victoria. Melbourne, Department of Human Services: Public Health and Development Division.
McKissock, D. M. and M. McKissock (1998). Bereavement counselling: Guidelines for practioners. Adelaide, Griffin Press.
Nurberger, J. I. and E. S. Gerson (1992). Genetics. Handbook of affective disorders. E. S. Payhel. Edinburg, Churchill Livingstone.
Parker, G. (1992). Early environment. Handbook of affective disorders. E. S. Payhel. Edinburgh, Churchill Livingstone: 171-184.
Parker, G. and H. Brotchie (1996). Psychomotor change as a feature of depressive disorders: historical overview and current assessment strategies. Melancholia: a disorder of movement and mood. G. Parker. Cambridge, Cambridge University Press.
Parker, V., A. H. C. Wong, et al. (2001). "Adverse reactions to St John's Wort." Canadian Journal of Psychiatry 46(1): 77-80.
Paul, G. L. (1967). "Strategies of outcome research in psychotherapy." Journal of consulting psychology 31: 109-118.
Payhel, E. S. and Z. Cooper (1992). Life events and social stress. Handbook of affective disorders. E. S. Payhel. Edinburgh, Churchill Livingstone.
Porter, R. (1997). The greatest benefit to mankind: a medical history of humanity from antiquity to the present. London, Harper Collins Publishers.
Ratay, J. J. and C. Johnson (1997). Shadow syndromes. London, Bantam Press.
Saraswati, K. (1983). Yogic management of common diseases. Bihar, Bihar School of Yoga.
Seligman, M. E. P. (1994). Learned optimism. Sydney, Random House.
Teicher, M. H. (2002). "Scars that won't heal: the neurobiology of child abuse." Scientific American 286(3): 54-61.
Turner, R. J. and B. Wheaton (1995). Checklist measurement of stressful life events. Measuring stress: a guide for health and social scientists. S. Cohen, R. C. Kessler and L. U. Gordon. New York, Oxford University Press: 29-58.
Wolman, B. B. (1973). Dictionary of behavioural science. New York, Van Nostrand Reinhold Company.
Yapko, M. D. (1994). When living hurts: directives for treating depression. New York, Brunner.
Yapko, M. D. (1999). Hand me down blues. New York, Golden Books.
Home Bob Rich's writing showcase Mudsmith site On depression and drugs
A popular self-help book A book of 50 case studies Bobbing Around
 As for vulnerability, the three environmental toxicity factors are acknowledged to interplay with one another. Interventions in this domain may focus on changing the environment or working through the consequences. The interplay between all these factors is graphically represented in figure 1.
As for vulnerability, the three environmental toxicity factors are acknowledged to interplay with one another. Interventions in this domain may focus on changing the environment or working through the consequences. The interplay between all these factors is graphically represented in figure 1.
 Figure 2 illustrates this interplay between vulnerabilities and the toxicity in the environment. The y-axis indicates the severity of symptoms with the horizontal line representing the threshold for clinical depression. The first dotted line (A) represents someone clinically depressed, the second (B) someone sub-clinically depressed (that is someone with a number of the symptoms of depression but not sufficient for a diagnosis of depression) and the third one (C) someone unlikely to have depressive features. Movements along the x-axis illustrate an increasing extent of the vulnerability component in the mix of an individual's combination of vulnerability and environmental toxicity in their observed presentation.
Figure 2 illustrates this interplay between vulnerabilities and the toxicity in the environment. The y-axis indicates the severity of symptoms with the horizontal line representing the threshold for clinical depression. The first dotted line (A) represents someone clinically depressed, the second (B) someone sub-clinically depressed (that is someone with a number of the symptoms of depression but not sufficient for a diagnosis of depression) and the third one (C) someone unlikely to have depressive features. Movements along the x-axis illustrate an increasing extent of the vulnerability component in the mix of an individual's combination of vulnerability and environmental toxicity in their observed presentation.
